Domestic resource mobilization (DRM) is the process through which countries raise, allocate, and spend their own funds to finance public services, including health. DRM is key to country ownership and ensuring sustainable financing for social services. DRM is often discussed in the context of increasing tax revenue, but financial resources for health can be mobilized from many other sources as well, including insurance premiums, user fees, the private sector, and through efficiency gains.
In recent years, DRM has taken a central role in global dialogue around development aid, particularly as external resources to support national-level activities decline while the costs of achieving development goals rise. In order to mobilize additional funding to meet global goals, such as the FP2020 commitments, donors and recipient countries agreed to the Addis Ababa Action Agenda in 2015, which includes commitments to DRM through widening the tax revenue base, improving tax collection, and combatting tax evasion and illicit financial flows.
Many external funders, including USAID, multilateral organizations, and private foundations, are working in conjunction with national level policymakers to explore ways to leverage finite resources to incentivize greater domestic resources for health. This includes investments in evidence-based advocacy, improved technical efficiency, tax policy, and innovative mechanisms to engage the private sector (including reducing fragmentation and changing provider incentives). Also, some donors (e.g., GAVI and the Global Fund) include explicit domestic cofinancing requirements as a condition to receive grants.
Need for DRM for Family Planning
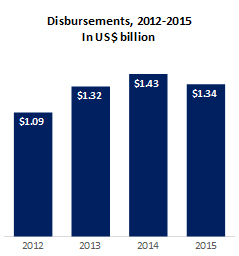
Source: Kaiser Family Foundation analysis of donor funding for family planning.
Mobilizing domestic resources will be critical to closing the resource gap, meeting unmet need, and ensuring sustainable, scaled financing for family planning. A recent analysis by the Reproductive Health Supplies Coalition found that low- and middle-income countries face a US$793 million funding gap for contraceptive supplies from 2018 to 2020 if new resources are not mobilized.
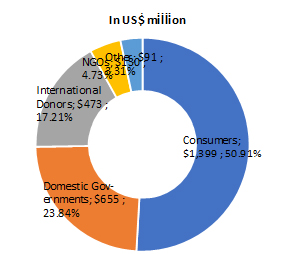
Source: The International Family Planning Expenditure Tracking Expert Advisory Group, based on estimates from Kaiser Family Foundation, UNFPA/NIDI, DHS, PMA2020, and Track20.
Like resources for health generally, external funds for family planning have plateaued (Figure 1). In 2015, donor governments spent US$1.34 billion on bilateral family planning programs. In FP2020 countries, out-of-pocket and government spending are responsible for an estimated three-quarters of family planning expenditures (Figure 2). This high dependency on out-of-pocket spending – coupled with stagnant or declining external financing – poses a risk to equitable and sustained access to family planning services, particularly for the poor. Mobilizing domestic resources through the government and private sector, and targeting these resources to those most in need has the potential to fill funding gaps and address financial barriers to access.
External funders can play a role in mobilizing domestic resources for family planning by investing in evidence generation, budget advocacy, or other activities that could lead to greater domestic investment in family planning. At the July 2017 FP2020 Summit, countries and donors, including USAID, committed to family planning financing solutions through increased domestic allocations and innovative new funding streams, including “catalytic” investments for DRM.
How Can Countries Mobilize Domestic Resources for Family Planning?
Domestic resources for family planning can come from many sources and mechanisms, as discussed below.
The Global Financing Facility
The World Bank-led Global Financing Facility (GFF) is a new financing mechanism that aims to increase domestic resources for maternal and reproductive health, including family planning. The GFF provides grants and loans to support countries in using existing resources more efficiently as well as to increase the total resources available through both tax-based financing as well as other sources, including the private sector. More information on the GFF is available on this website.
Government Tax Revenues
The government raises revenue through imposing a variety of taxes on income and goods and services. Increasing tax revenue by widening the tax base or improving tax collection makes additional resources available for government spending. In order for increased tax revenue to benefit family planning, these additional resources need to be partially or fully allocated to family planning in the government budget.
Several countries have increased allocations to family planning in government budgets at both national and subnational levels through targeted advocacy. In Guatemala, the government implemented a 15 percent tax on alcohol, which it then earmarked for family planning. In Senegal, mayors were given the authority to budget for family planning in 2014. A network of women’s rights organizations engaged in targeted, local advocacy and, as a result, 64 mayors budgeted US$125,000 for family planning from 2014 to 2017. In Malawi, high-level political commitment to family planning with civil society organization advocacy resulted in the government increasing its funding for contraceptives by 17 percent from 2015 to 2016.
Efficiency Gains
DRM can also take the form of using existing resources more efficiently. Poor budget execution (e.g., not spending the full allocation of funds), overpaying for commodities, corruption, and inappropriate mix of health staff are all sources of inefficiency. Improving management and use of resources allows countries to achieve more with what they have. For example, several countries have shifted provision of certain family planning methods to lower-level cadres of health workers in order to optimize use of the health workforce for family planning, reduce costs, and improve accessibility of services.
Health Insurance Schemes
Insurance schemes can mobilize resources for family planning if family planning is included in the benefits package. Many countries in Latin America, for example, have incorporated family planning in their general universal health coverage efforts, including making it part of insurance benefits packages. This has helped expand family planning coverage while reducing the financial burden for accessing services. More information on health insurance and family planning is available on this page.
Private Sector
The private sector broadly includes health service providers, investors and philanthropic organizations, pharmaceutical producers, distributors, wholesalers and retailers, and private firms. These actors can expand domestic resources available for family planning in a number of ways, including providing services and commodities as well as capital investments. DRM efforts should facilitate these contributions. For example, governments can ensure that private providers can access family planning commodities and consumables at reasonable prices. If private providers are able to attract and retain users with the ability to pay for family planning, even at subsidized prices, governments can better target their resources to those who are less able to pay. Identifying promising opportunities for this kind of private sector engagement requires an evidence-based process to identify market players and understand how they can contribute to improved access to family planning, referred to as a total market approach. More information on a total market approach for family planning is available on this page.
Resources
Le but de cette note est de fournir des mesures pratiques que les législateurs peuvent prendre pour améliorer la durabilité du financement de la
The purpose of this guide is to provide practical action steps that MOF staff can take to improve the sustainability of family planning financing
Le but de ce document est de fournir des mesures pratiques que le personnel du programme de planification familiale du MS peut prendre pour
The purpose of this brief is to provide practical action steps that MOH family planning program staff can take to improve the sustainability of
The purpose of this brief is to provide practical action steps that legislators can take to improve the sustainability of family planning
This guide is intended to help countries identify and implement catalytic interventions for domestic financing of family planning across four
Senegal's family planning program remains significantly dependent on external resources and struggles with funding activities outlined in the
Community health workers provide essential care to many populations and are a vital component of most community health programs in Africa. This
The health system in Mali relies on community health workers to deliver essential services to rural populations, however, the program is almost














