Millions around the world lack access to affordable, high-quality health services, resulting in poor health outcomes and catastrophic out-of-pocket healthcare expenditures that exacerbate poverty. Universal health coverage (UHC) refers to the concept that everyone can access the health services and commodities they need without financial hardship. UHC has become a global movement, evidenced by the formation of the UHC2030 partnership and inclusion of UHC in the Sustainable Development Goals.
While an aspirational concept, progress toward UHC is measurable. The goals are to expand the types of services available, the populations covered (i.e., the proportion of a population in need of a service who access it), and protection from financial risk in a way that promotes equity and optimizes health outcomes (Figure 1). Underlying UHC is a focus on equity and quality service delivery. Countries will have different pathways toward UHC due to differences in their health priorities and demographic, epidemiological, geographic, and economic profiles. Thus, countries are developing UHC roadmaps that are unique to their context.
Figure 1. Dimensions of UHC
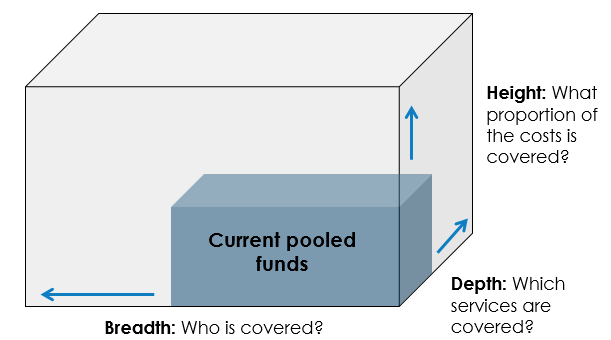
Source: Adapted from WHO. 2010.
To achieve UHC requires approaches that go beyond the health sector: countries will need multisectoral approaches that improve infrastructure, education, agriculture, social welfare, and other areas that have direct or indirect impacts on health. Within the health sector, countries will need to strengthen all aspects of the health system—including the health workforce, infrastructure, information systems, governance, the supply chain, financing, and service delivery—to meet the evolving health needs of their populations.
Health financing is particularly relevant to UHC if countries are to finance healthcare for all while protecting individuals and households from undue financial hardship. While mobilizing additional resources for health is important, countries also need to maximize the use of existing funding and redistribute resources to allow for cross-subsidization (i.e., the rich subsidize the poor and the healthy subsidize the sick). There are multiple health financing approaches and mechanisms that can advance UHC. Health insurance is often associated with UHC as it can potentially result in increased resources for health, cross-subsidization through pooling of funds, and efficient purchasing of health services. However, health insurance is not the only option and may not be appropriate in certain country contexts. For example, countries with large proportions of the population living in poverty and working in the informal sector may face difficulties enrolling people in health insurance schemes and identifying those who need insurance subsidies. These issues are explored elsewhere on this website.
Why Is UHC Important for Family Planning?
In a country that has achieved UHC, women and their partners who want to use family planning should have access to a range of affordable family planning methods across a range of providers. However, many countries still have a long way to go before achieving UHC, and family planning may not be considered by key stakeholders when designing, introducing, or scaling up UHC schemes. Therefore, champions need to reinforce the importance of family planning links to broader UHC reforms in a country and advocate for it being included in the design and implementation of these reforms. The three dimensions of UHC (Figure 1) offer a useful framework for assessing how well a country is including family planning in UHC schemes:
-
Who is covered? Certain segments of a population, such as the poor, youth, or indigenous groups may face greater barriers than others in accessing family planning services but are also not sufficiently included in efforts to expand access to services. For instance, an insurance scheme may cover the full cost of family planning services, but if certain populations are largely uninsured, they will not benefit. Further, nonfinancial barriers to access, such as sociocultural norms that limit women’s autonomy in reproductive health decision making, may need to be addressed in order to reduce inequities in access and effectively reach more women and their partners with family planning services.
-
What services are covered? Family planning providers may offer a limited set of methods due to lack of supplies, inadequately trained providers, and other barriers. These constraints can result in limited method choice. In order to expand the types of family planning services available at an affordable price, financing for UHC—including government budgeting for health, benefits packages, performance-based financing, and contracting with private providers—needs to include a diverse set of family planning methods and services.
-
What proportion of the costs is covered? Many countries provide family planning commodities in public facilities free of charge, which may promote uptake of family planning services. However, some women may not be able to afford other costs associated with accessing family planning services, such as transportation or the user fee for consulting a provider. Initiatives such as voucher programs could help subsidize these costs. UHC reforms should also consider who has the ability and willingness to pay for family planning services, which will allow targeting of limited financial resources to those most in need.
Examples of Consideration of Family Planning in UHC Schemes
Ghana launched its National Health Insurance Scheme (NHIS) in 2003. It is one of the most ambitious UHC-oriented schemes in Africa. While NHIS has resulted in rapid health insurance enrollment and increased utilization of antenatal and delivery care, it only covers about 40 percent of the population and caters to wealthier populations through its flat-rate premiums. Thus, the financial sustainability of the scheme continues to pose a challenge. Further, NHIS does not cover family planning methods in its benefits package, which means that insured women and their partners must pay out of pocket to access family planning services. However, lessons learned in designing and implementing NHIS can be applied to other countries considering their options for reaching UHC. One such lesson is the need for early engagement and concerted advocacy by family planning stakeholders with the ministry of health, parliament, health insurance authorities, and others to ensure inclusion of family planning in the design of UHC schemes.
In contrast, Indonesia has included family planning in the benefits package of its national health insurance scheme, Jaminan Kesehatan Nasional (JKN), since its inception in 2014. Family planning counseling, methods, and management of side effects are all covered in the benefits package. Still, challenges remain, as many women, including poor women, are not covered by JKN and may pay out of pocket for family planning services. Of the 13.5 million family planning users in the bottom wealth quintile, less than 60 percent are covered by JKN. The government is working with partners to address these issues and scale up coverage.
Resources
The following website is the theme resource page on family planning and universal health coverage. It is a curation of resources, evidence,...








